⚡ Quick Answer
While diabetes doesn’t discriminate based on gender, women face specific risks and challenges. Several factors make women uniquely susceptible to diabetes:
Introduction to Diabetes in Women
When we discuss health conditions that affect millions globally, diabetes is often at the forefront. But did you know that women experience a unique set of challenges and symptoms related to this disease? The intricate interplay between female physiology, hormones, and diabetes makes understanding this condition essential for every woman. Whether you’re a young adult or in your golden years, being informed about diabetes can make a significant difference in early detection, management, and overall quality of life.
What is Diabetes?
Imagine our body as a car engine, and glucose (a type of sugar) as the fuel. For our engine to run smoothly, it needs a regulated supply of this fuel. Diabetes is essentially a disruption in this supply chain. Our body either doesn’t produce enough of a hormone called insulin, which is responsible for helping glucose enter our cells, or it can’t use the insulin it does produce effectively. When this happens, the glucose stays in our bloodstream, leading to elevated blood sugar levels. Over time, if not managed, this can damage various body parts, including the heart, kidneys, eyes, and nerves. There are primarily two types of diabetes: Type 1, where the body doesn’t produce insulin, and Type 2, where the body doesn’t use insulin properly. There’s also gestational diabetes, which some women develop during pregnancy.
Why Women are at Risk
While diabetes doesn’t discriminate based on gender, women face specific risks and challenges. Several factors make women uniquely susceptible to diabetes:
- Hormonal Fluctuations: The monthly menstrual cycle means that women experience regular hormonal fluctuations. These hormonal changes can affect insulin sensitivity, leading to temporary spikes in blood sugar levels.
- Pregnancy: Gestational diabetes is a condition that arises during pregnancy. Though it usually resolves post-delivery, it increases the risk of developing Type 2 diabetes later in life.
- Polycystic Ovary Syndrome (PCOS): Women with PCOS have a higher risk of insulin resistance. PCOS, coupled with other factors like obesity, can increase the chances of developing diabetes.
- Menopause: As women undergo menopause, changes in hormone levels can lead to weight gain and decreased insulin sensitivity, both of which are risk factors for diabetes.
Detailed Symptoms
10. Frequent Urination: The Silent Alarm

Securing the tenth spot is the often-misunderstood symptom, Frequent Urination. You might notice an unexplained increase in your restroom visits. Many tend to overlook this, thinking it’s due to increased fluid intake or colder weather conditions.
Understanding Polyuria
The clinical term for this phenomenon is ‘polyuria.’ When there’s an excess of sugar in the bloodstream, our kidneys work overtime to filter and absorb this surplus glucose. If they can’t manage, the extra sugar gets expelled through urine, leading to increased bathroom trips.
Research Insights
A revealing study in 2015 from the Journal of Clinical Endocrinology and Metabolism highlighted this issue. It found that a significant 46% of early-diagnosed diabetic women flagged frequent urination as their first noticeable symptom. This sign extends beyond mere frequency; the volume of urine might also rise, sometimes even resulting in unintentional weight loss from fluid loss.
9. Blurred Vision: A Veiled Warning
Earning its place at number nine, Blurred Vision is a symptom that many misinterpret. Those prolonged hours staring at screens might make the world seem out of focus momentarily. While it’s tempting to dismiss this as typical digital eye strain, consistent episodes of blurred vision can indicate deeper issues.

The Diabetes Connection
Persistent high blood sugar levels can lead to the eye’s lens swelling, affecting our ability to see clearly. The American Diabetes Association brought to light a concerning fact: diabetes is the main reason for new blindness cases in adults aged 20 to 74.
The Bigger Picture
Further deepening our understanding, a 2017 research piece in Diabetes Research and Clinical Practice discussed the link between sustained high blood sugar and conditions like diabetic retinopathy, a significant cause of vision deterioration.
8. Fatigue: Not Just Your Regular Tiredness

Fatigue, as understood in the diabetes sphere, goes beyond mere weariness at the end of a long day. Imagine feeling perpetually drained, even if your activities were mundane? This profound, relentless fatigue is a pivotal sign of diabetes.
The Science Behind the Fatigue
When there’s a surge in blood sugar levels, cells don’t receive the glucose needed for energy. This forces the body to use muscle and fat for its energy needs, leading to an overall feeling of exhaustion.
Numbers Speak Louder
To shed more light on the significance of this symptom, the American Diabetes Association shared a statistic: an alarming 61% of women with undiagnosed type 2 diabetes report intense fatigue. Recognizing this symptom is crucial for early diagnosis and effective management.
7. Increased Hunger: More Than Just an Appetite
Positioned notably at number 7, we delve into a sensation that’s frequently brushed aside: Increased Hunger. While an occasional surge in appetite after an intense workout is expected, when it becomes a consistent trait, it’s essential to consider the underlying causes.

Hunger and Diabetes
Here’s the paradox of diabetes: you have an abundance of glucose circulating in the bloodstream, yet not enough makes its way into the cells that need it. As a result, these starved cells send out distress signals, prompting the body to ingest more food, and thus more glucose. This miscommunication results in persistent hunger.
The Hormonal Influence
A captivating study from the Journal of Endocrinology and Metabolism brought to light that a significant 38% of women in the early diabetes phase experienced unexplained hunger spikes. In women, this symptom can be accentuated due to hormonal fluctuations, especially during their menstrual cycles. It’s not just a simple craving; it’s the body’s way of alerting about an impending energy crisis.
6. Reduced Sensation: The Silent Alert
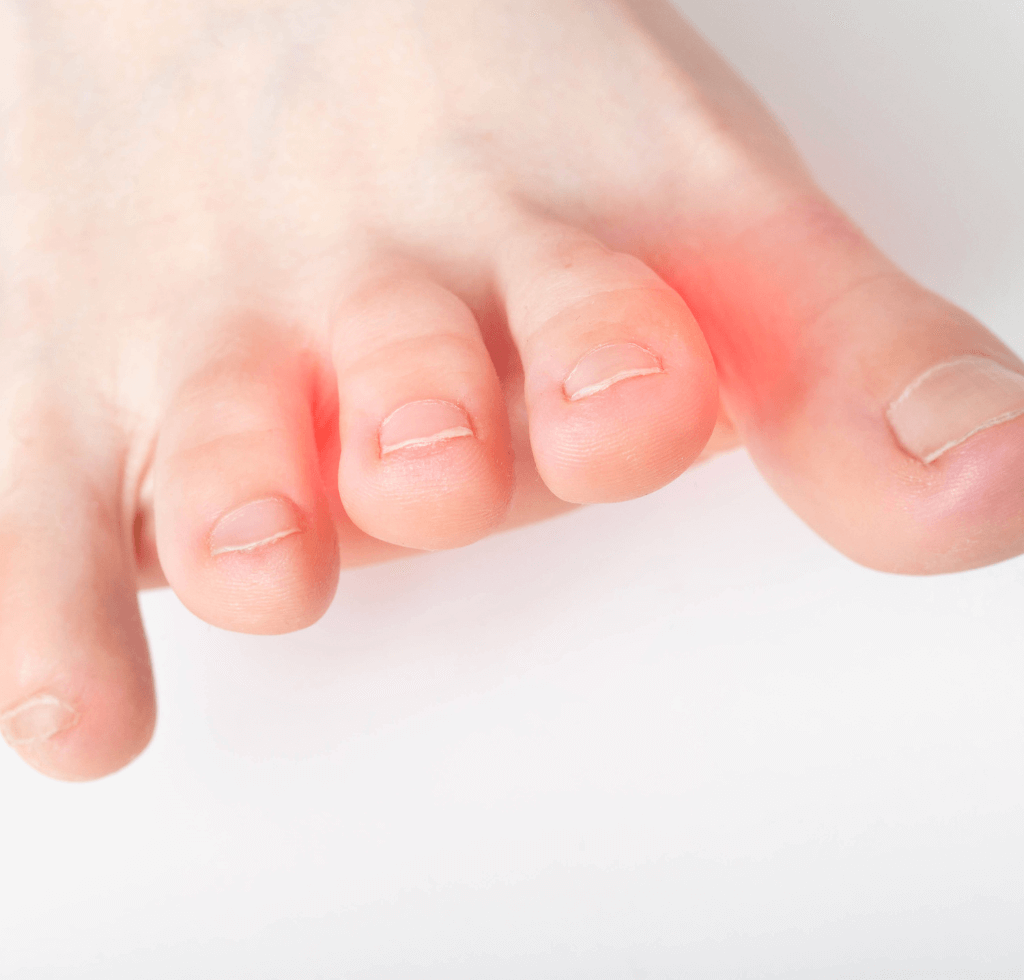
Capturing the sixth position, Reduced Sensation is an enigma. Often, it’s the extremities, like fingers and toes, that bear the brunt, experiencing a decreased sense of touch or even a peculiar tingling.
Understanding Diabetic Neuropathy
Persistently high blood sugar levels can inflict harm on the body’s nerve fibers, leading to a condition known as diabetic neuropathy. The manifestations can range from mild numbness to severe pain.
A Common Underestimate
Interestingly, data from the National Institute of Diabetes and Digestive and Kidney Diseases unveiled that approximately 30% of diabetic women exhibited signs of peripheral neuropathy, even before being officially diagnosed. Such subtle signs, especially in women, can be misattributed to factors like wearing tight shoes or cold temperatures. Recognizing this symptom can pave the way for early interventions, potentially preventing aggravated nerve damage.
5. Skin Changes: The Body’s Canvas Speaks
Claiming the fifth spot, we turn our focus to the body’s largest organ: the skin. Often, the skin acts as a mirror, reflecting internal health conditions, and in the context of diabetes, it’s no different.

Telltale Signs
Diabetic individuals, especially women, might notice peculiar dark patches in skin fold areas like the neck or underarms, medically termed acanthosis nigricans. Additionally, diabetic dermopathy can lead to the emergence of shiny, scaly patches, often mistaken for age-related skin changes.
Skin and Diabetes
Highlighting the significance of this symptom, a study published in the Journal of the European Academy of Dermatology and Venereology reported that a staggering 50% of diabetic individuals would face skin-related issues during their lifetime. For many women, these skin alterations might be dismissed as mere aesthetic concerns. However, they serve as crucial indicators of underlying glucose imbalances, emphasizing the need for prompt medical attention.
4. Unexplained Weight Loss: The Paradox of Diabetes

Taking the fourth spot is the perplexing symptom, Unexplained Weight Loss. At first glance, it seems almost ironic. Diabetes, a condition intertwined with high blood sugar, leading to weight loss? But the body’s rationale behind this is deeply rooted in its metabolic processes.
The Underlying Biology
Here’s the deal: when the body is unable to utilize glucose for energy, primarily due to insulin inefficiency, it resorts to an alternative source. It begins metabolizing fat and muscle for energy, causing a noticeable reduction in weight.
A Statistic to Ponder
Highlighting the gravity of this symptom, data from the Centers for Disease Control and Prevention revealed an intriguing statistic. About 40% of women, prior to their official diabetes diagnosis, noted a sudden weight reduction spanning a few months. While any unexpected drop in weight might seem like a cause for celebration for some, understanding its root cause is crucial. It might be the body’s subtle way of raising a red flag.
The Body’s Narrative
The myriad symptoms, particularly in women, underscore the body’s intricate communication methods. Delving deeper into this narrative brings forth the necessity for vigilance and proactive health decisions. Here’s a tantalizing thought: Among the forthcoming symptoms, one is closely related to women’s reproductive health. It’s frequently misdiagnosed due to its resemblance to another prevalent condition. Intrigued? Stay with us as we unravel the top signs and answer this captivating query.
3. Yeast Infections: More Than Just a Nuisance
Claiming the third position, Yeast Infections might seem like a mere bothersome ailment to many women. However, their recurrent presence can be a significant indicator pointing towards diabetes.

Diabetes and Yeast: The Connection
Elevated blood sugar levels present a unique challenge for women. The heightened glucose concentration in vaginal secretions becomes a breeding ground for yeast, allowing it to thrive. But there’s more: persistent high sugar levels can weaken the immune system, impairing its ability to fend off these infections.
A Research Insight
Shedding light on this issue, an enlightening study from Clinical Microbiology Reviews delivered a stark revelation. Diabetic women grapple with yeast infections nearly twice as often as their non-diabetic counterparts. This statistic underscores the importance of perceiving recurrent yeast infections not just as isolated events but as potential indicators of underlying glucose imbalances. Recognizing these signs early can pave the way for timely interventions and holistic health management.
2. Urinary Tract Infections (UTIs): Beyond Simple Inconvenience
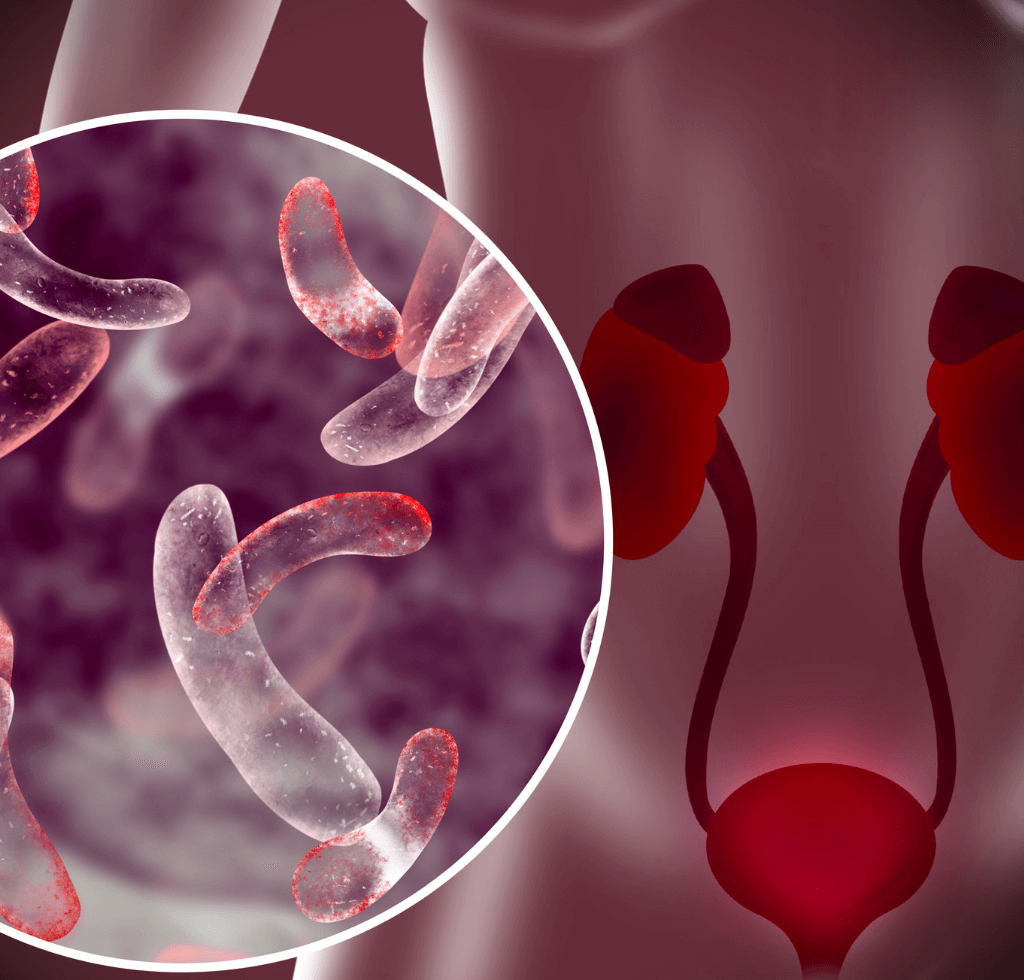
Moving forward to our second spot, we tackle Urinary Tract Infections, commonly known as UTIs. While UTIs are a frequent complaint among many women, their association with diabetes often goes unnoticed.
The Diabetes-UTI Connection
The intertwining of UTIs and diabetes is more intricate than one might assume. Persistently elevated blood sugar levels can diminish the immune system’s efficacy, making it challenging to ward off infections. Additionally, the surplus sugar present in the urine can transform the bladder into a welcoming haven for detrimental bacteria.
A Revealing Study
Shedding light on this association, a detailed study published in the Journal of Urology presented a concerning revelation. Diabetic women face a heightened risk, up to 60% more, of contracting UTIs in comparison to women without diabetes. Such recurrent UTIs aren’t just a source of pain and discomfort; they might be echoing the silent alarms of sustained high sugar levels, urging for a comprehensive health assessment.
The Interconnected Body
The frequent occurrence of UTIs in diabetic women emphasizes our body’s intricate web of systems. Viewing them not merely as isolated conditions but as potential harbingers of a deeper underlying issue is crucial. However, our most crucial sign awaits. Are you prepared for the grand revelation?
1. Polycystic Ovary Syndrome (PCOS): The Silent Symphony of Symptoms

Securing the paramount position on our list is the multifaceted condition: Polycystic Ovary Syndrome, widely recognized as PCOS.
Beyond Reproductive Health
PCOS transcends the realm of mere reproductive concerns. It’s a multifarious endocrine disorder that casts its shadow on countless women globally. Intriguingly, the villain in both the PCOS and diabetes narratives remains consistent: insulin resistance. PCOS-afflicted women tend to produce insulin in quantities exceeding the norm. This insulin surplus can prompt the ovaries to release heightened levels of androgens, such as testosterone, culminating in symptoms like irregular menstruation, excessive hair growth, and the characteristic ovarian cysts.
The PCOS-Diabetes Intersection
But where does diabetes intersect with the PCOS storyline? A pioneering research article from the Journal of Clinical Endocrinology & Metabolism divulged that PCOS-stricken women face a risk fourfold higher of developing type 2 diabetes relative to those without the syndrome. More alarmingly, this vulnerability isn’t restricted to later life stages. Symptoms indicative of diabetes can surface in PCOS women as early as their third decade of life.
Furthermore, the PCOS Awareness Association has highlighted a concerning statistic: approximately half of all PCOS women are either overweight or obese. This added weight can further accentuate insulin resistance, establishing a vicious cycle that intensifies the manifestations of both PCOS and diabetes.
A Beacon of Hope
Yet, amidst these complexities, a glimmer of hope persists: proactive detection and management can markedly shift the PCOS trajectory. Implementing dietary modifications, managing weight, and certain therapeutic interventions can assist in reestablishing hormonal equilibrium and augmenting insulin responsiveness.
The Body’s Melodious Dance
Deciphering the enigma of PCOS underscores the delicate balance and intricate dialogues within our body. Recognizing and responding to these nuanced patterns, especially in multifactorial conditions like PCOS, can be transformative. Through today’s journey, our aspiration is not just to impart knowledge but to empower you to attune to and champion your body’s unique symphony.
Proactive Measures for Diabetes
Understanding Before Acting
Before diving into the preventive measures, it’s vital to comprehend that diabetes, particularly type 2, can often be managed and sometimes even prevented with some lifestyle adjustments. Early detection, combined with proactive measures, can significantly reduce the risk of complications.
Dietary Disciplines
- Balanced Meals: Incorporate a mix of proteins, fats, and carbohydrates in every meal. Opt for whole grains, lean proteins, and healthy fats to ensure blood sugar stability.
- Limit Sugars and Saturated Fats: Reducing the intake of sugary beverages and snacks, along with saturated fats, can play a pivotal role in maintaining a healthy blood sugar level.
- Stay Hydrated: Drinking ample water aids in maintaining a healthy blood sugar level and helps the kidneys flush out excess sugar.
Stay Physically Active
- Regular Exercise: Engaging in physical activity, like brisk walking, swimming, or cycling, for at least 150 minutes a week can enhance insulin sensitivity.
- Strength Training: Incorporate resistance training into your routine. It aids in building lean muscle mass, which can help regulate blood sugar.
Regular Health Check-ups
- Routine Screenings: Periodic blood sugar testing can detect potential issues before they escalate.
- Stay Informed: Keep abreast of the latest research and recommendations regarding diabetes management.
Lifestyle and Mental Well-being
- Stress Management: Chronic stress can elevate blood sugar levels. Techniques like meditation, deep breathing exercises, and yoga can be beneficial.
- Adequate Sleep: Aim for 7-9 hours of sleep each night. Quality sleep is crucial for insulin sensitivity and overall health.
Redefining Conclusions: Wrapping it Up
As we conclude our deep dive into the signs of diabetes in women, it’s essential to understand that knowledge is the first step towards empowerment. Recognizing symptoms, understanding their implications, and taking proactive measures can redefine one’s health trajectory. Remember, every individual’s journey is unique, and while this guide provides a comprehensive overview, personal experiences may vary.
For a more visual understanding, we encourage you to watch this informative video. The knowledge imparted can offer a deeper insight into managing and understanding diabetes:
FAQs
- What is the primary difference between type 1 and type 2 diabetes?
Type 1 diabetes is an autoimmune condition where the body doesn’t produce insulin. Type 2 diabetes is more common and is characterized by the body’s inability to use insulin effectively. - Can diabetes symptoms be reversed?
While some symptoms and complications can be managed or even alleviated with appropriate treatment and lifestyle changes, diabetes itself is a chronic condition. - How often should I get screened for diabetes?
It’s recommended to have a routine blood sugar test every three years, starting at age 45. However, if you have risk factors or symptoms, more frequent testing might be necessary. - Is diabetes hereditary?
Both type 1 and type 2 diabetes have a genetic component. However, lifestyle factors play a significant role, especially in type 2 diabetes. - Can I prevent diabetes entirely?
While genetic factors can’t be changed, adopting a healthy lifestyle can significantly reduce the risk of developing type 2 diabetes. Regular check-ups, a balanced diet, and physical activity are critical components of prevention.
📖 Related Articles You Might Enjoy
- 5 Breakfast Hacks That Turn Off Insulin Resistance (Eat Before 8am)
- 7 Foods DESTROYING Your Pancreas Every Morning
- 7 Meats You Should NEVER Eat If You Have Diabetes
- 10 Eyesight-Saving Habits for Diabetics (Most People Skip #3!)
🌐 From Our Health Network:
📚 Sources & References
This article is based on information from the following trusted medical sources:
⚕️ Medical Disclaimer
This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or qualified health provider before making changes to your diet, exercise, or treatment plan. The information presented here is based on peer-reviewed research and should not be used for self-diagnosis. If you are experiencing a medical emergency, call your local emergency services immediately.









