⚡ Quick Answer
Understanding how diabetes affects your body and what medication options are available to you is essential in your journey towards effective diabetes management.
Understanding how diabetes affects your body and what medication options are available to you is essential in your journey towards effective diabetes management. This article aims to provide insight into the top 5 diabetes medications for seniors and give you the knowledge to discuss these options with your healthcare provider.
Understanding Diabetes
Diabetes is a chronic condition that affects the body’s ability to process sugar or glucose. It results in higher than normal blood sugar levels (ADA blood sugar targets), which over time can lead to serious health complications. Diabetes is mainly categorized into two types: Type 1 and Type 2.
Type 1 Diabetes (CDC Type 1 diabetes)
Type 1 diabetes is an autoimmune condition where the body’s immune system mistakenly attacks the insulin-producing cells in the pancreas. This results in the body producing little to no insulin, a hormone that’s vital in allowing glucose to enter cells and be used for energy. This form of diabetes, often diagnosed in children and young adults, requires daily insulin intake.
Type 2 Diabetes (CDC Type 2 diabetes)
In contrast, Type 2 diabetes is more common and usually develops in people over 45. In this case, the body either resists the effects of insulin or doesn’t produce enough to maintain normal glucose levels. While lifestyle factors like obesity (CDC obesity) significantly increase the risk of Type 2 diabetes, genetics can also play a role. Management usually involves lifestyle changes and, often, medication.
Necessity of Medication in Diabetes Management
While diet, exercise, and maintaining a healthy weight play crucial roles in managing diabetes, medication is often necessary, especially as the disease progresses. Let’s explore the importance of insulin and the role of oral medications.
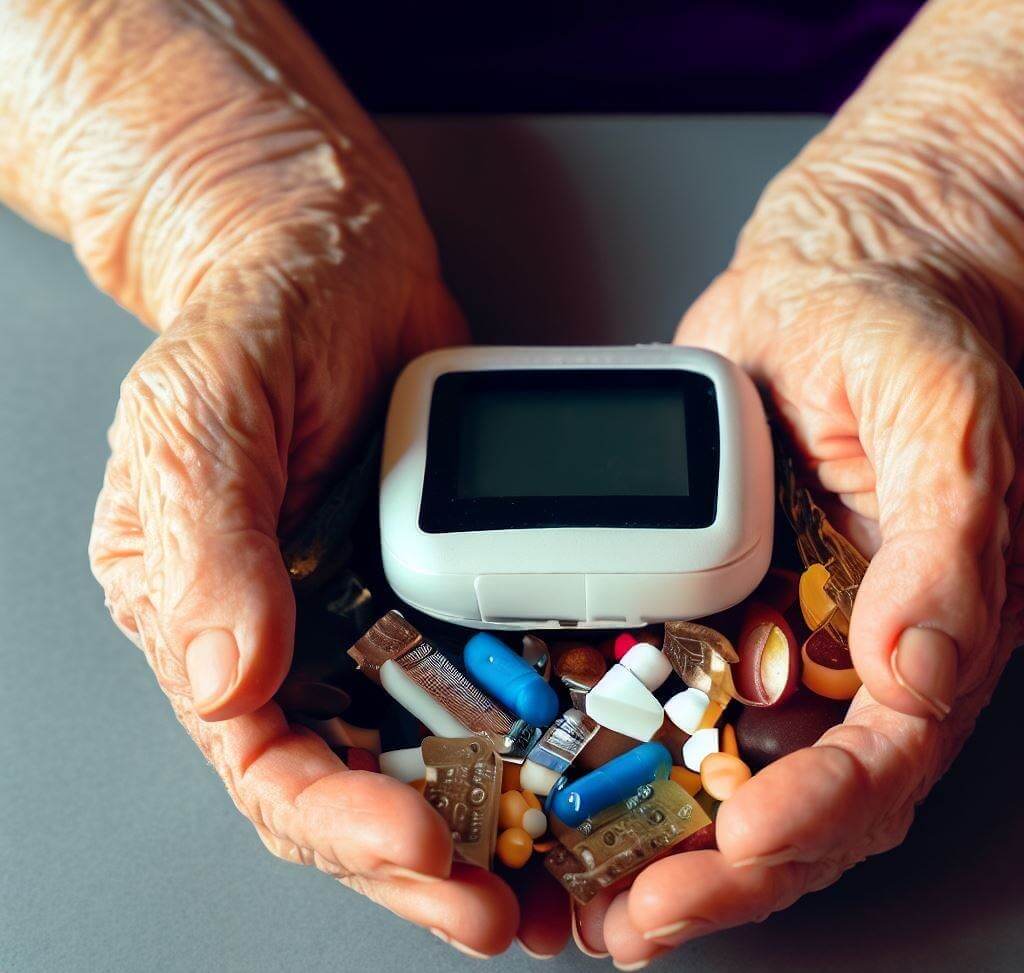
Importance of Insulin
Insulin is the key hormone that allows cells to take in glucose and use it as fuel. Without it, glucose accumulates in the blood, leading to high blood sugar levels. For those with Type 1 diabetes, insulin injections are a lifeline as their bodies cannot produce it. For Type 2 diabetes patients, insulin therapy may become necessary if other medications can’t control blood sugar levels adequately.
Role of Oral Medications
Oral medications are often the first line of treatment in managing Type 2 diabetes, along with lifestyle changes. These medications work in various ways, from stimulating the pancreas to produce more insulin, reducing glucose release from the liver, to improving insulin sensitivity (NIDDK insulin sensitivity) in cells. As diabetes is a progressive disease, many patients may eventually need a combination of drugs to effectively manage their condition.
Top 5 Diabetes Medications for Seniors
There are several medications available for diabetes management. However, certain ones are often recommended for seniors due to their efficacy, tolerability, and lower risk of causing hypoglycemia (NIDDK), a condition characterized by dangerously low blood sugar levels. Here are the top five:
Metformin (MedlinePlus: metformin)
Metformin is usually the first medication prescribed to those with Type 2 diabetes. It works by reducing the amount of glucose your liver releases into the blood and improving insulin sensitivity. This drug has been around for many years and is recommended by various guidelines due to its long-term safety and efficacy.
Pros and Cons of Metformin
- Pros
- Established safety and efficacy record
- May contribute to modest weight loss
- Low risk of hypoglycemia
- Cons
- Potential side effects include digestive issues like nausea and diarrhea
- Not suitable for people with severe kidney disease
- Rare but serious condition called lactic acidosis can occur
Sulfonylureas
Sulfonylureas, such as glipizide, glyburide, and glimepiride, stimulate the pancreas to release more insulin. They’re a group of older drugs but still commonly used due to their effectiveness.
Pros and Cons of Sulfonylureas
- Pros
- Proven effectiveness in lowering blood sugar
- Lower cost as many are available in generic form
- Cons
- Higher risk of hypoglycemia compared to other drugs
- Potential weight gain
- Not suitable for those with severe kidney disease
Please note that this is not medical advice and you should always consult your healthcare provider to discuss the best medication options for your individual situation. Let’s continue exploring more medication options in the next section.
DPP-4 Inhibitors
DPP-4 inhibitors, such as sitagliptin and linagliptin, work by increasing the levels of incretin hormones in the body, which in turn stimulate the release of insulin and reduce the production of glucagon, both leading to lower blood sugar levels.
Pros and Cons of DPP-4 Inhibitors
- Pros
- Lower risk of hypoglycemia as they act in a glucose-dependent manner
- Neutral effect on weight
- Few side effects, with the most common being mild and including symptoms such as runny nose and sore throat
- Cons
- Can be expensive as there are currently no generic versions available
- Rare, but severe joint pain may occur
- Not as potent in reducing HbA1c (NIDDK A1C test) levels compared to other classes of medications
GLP-1 Receptor Agonists (NIDDK insulin & medicines)
GLP-1 receptor agonists, like liraglutide and dulaglutide, mimic the functions of the body’s incretin hormones, stimulating insulin release in a glucose-dependent manner, delaying gastric emptying, and inducing satiety. These medications are injectable.
Pros and Cons of GLP-1 Receptor Agonists
- Pros
- Highly effective in reducing HbA1c levels
- Promote weight loss
- Low risk of hypoglycemia
- Cons
- Side effects may include nausea and vomiting, especially at the beginning of the treatment
- Not suitable for people with a history of pancreatitis or medullary thyroid carcinoma
- More expensive compared to older drugs
SGLT2 Inhibitors (NIDDK insulin & medicines)
SGLT2 inhibitors, such as empagliflozin and canagliflozin, work by blocking a protein in the kidneys, leading to the excretion of more glucose in urine and hence, lower blood glucose levels.
Pros and Cons of SGLT2 Inhibitors
- Pros
- Can lead to weight loss and blood pressure reduction
- Lower risk of major cardiovascular events and hospitalization for heart failure
- Cons
- Potential side effects include urinary tract infections and yeast infections
- May increase the risk of diabetic ketoacidosis (NIDDK), a serious condition
- Not recommended for those with severe kidney disease
It’s important to remember that the effectiveness of diabetes medications depends on individual factors including the stage of the disease, the person’s overall health, other co-existing health conditions, and their lifestyle. Please consult your healthcare provider before starting any new medication regimen.

Understanding Side Effects and Interactions
Given that seniors typically take multiple medications for various conditions, understanding potential side effects and drug interactions becomes even more essential. Some diabetes medications might interact with other drugs that seniors could be taking, like blood pressure medication, cholesterol medication, or anticoagulants. Such interactions could increase or decrease the effectiveness of either medication, leading to potentially harmful health consequences.
For instance, Metformin, despite being the first line of treatment for type 2 diabetes, can interact negatively with contrast dyes used in certain radiology procedures. Moreover, it might lead to lactic acidosis in some patients, especially those with impaired kidney function, which is more common among seniors. Consequently, doctors usually adjust Metformin doses based on a senior patient’s kidney function.
Similarly, Sulfonylureas could cause hypoglycemia or low blood sugar levels, especially when combined with certain other medications. Seniors, in particular, need to be cautious as they might not recognize the symptoms of hypoglycemia, such as dizziness, confusion, or shakiness, which can increase the risk of falls and other injuries.
DPP-4 inhibitors are generally well-tolerated but can cause joint pain in some patients. They could also potentially interact with other medications metabolized by the same liver enzymes.
GLP-1 receptor agonists may cause gastrointestinal side effects like nausea, vomiting, and diarrhea, especially when starting treatment or increasing the dose. They can also slow down the rate at which the stomach empties, which might affect the absorption of oral medications.
SGLT2 inhibitors might interact with diuretic medications and lead to dehydration. These medications can also increase the risk of urinary tract infections, which might be more common in senior women.
Besides these interactions, it’s worth mentioning that the same diabetes medication can affect seniors differently compared to younger adults. This is due to changes in the body associated with aging, such as decreased kidney and liver function, which can alter how the body metabolizes drugs. Hence, healthcare providers often adopt a ‘start low and go slow’ approach when prescribing diabetes medications to seniors.
Creating a Comprehensive Diabetes Management Plan
Understanding the medications is only part of the journey; integrating them into a comprehensive diabetes management plan is the key to successful diabetes management.
Such a plan should consider several factors, including lifestyle changes, dietary adjustments, physical activity, and regular blood sugar monitoring. For example, even simple changes like reducing the intake of processed foods, increasing the consumption of fruits and vegetables, and incorporating regular physical activity like walking or yoga can significantly improve blood glucose control.
However, each senior is unique, and so should be their diabetes management plan. A plan that works well for one person might not work for another. Thus, it’s crucial to work closely with healthcare professionals, such as doctors, dieticians, and diabetes educators, to create a plan that’s tailored to individual needs and preferences.
Remember, it’s not just about the medications. It’s also about understanding how different aspects of your lifestyle, including what you eat, how active you are, and how you handle stress, affect your blood sugar levels. Regularly monitoring blood sugar levels can provide valuable insights into how different factors influence them, helping you and your healthcare team make necessary adjustments to your diabetes management plan.
In essence, managing diabetes as a senior might seem daunting, but with a thorough understanding of the various medications available, their pros and cons, potential side effects, and interactions, coupled with a comprehensive diabetes management plan, it becomes much more manageable. It might take some time to find the right balance of medications and lifestyle changes, but the result is well worth the effort – a healthier, more fulfilling life.

Conclusion
Diabetes is a chronic condition that requires consistent management to maintain healthy blood sugar levels. For seniors, managing diabetes might seem overwhelming due to the numerous options of medications available. However, by understanding the basics of how different medications work, their benefits and potential drawbacks, you can have a more informed conversation with your healthcare provider about which medication regimen could be right for you. Remember, while medications play a crucial role in managing diabetes, a balanced diet, regular physical activity, and maintaining a healthy lifestyle are equally important.
In summary, Metformin, Sulfonylureas, DPP-4 inhibitors, GLP-1 receptor agonists, and SGLT2 inhibitors are commonly prescribed diabetes medications for seniors. Each comes with its unique mechanism of action, pros, and cons. What works best will vary from person to person, and a comprehensive and individualized treatment plan should be developed in consultation with healthcare professionals.
Living with diabetes might be challenging, but it’s certainly manageable. With the right medication, lifestyle adjustments, and a proactive approach, seniors can lead a healthy and fulfilling life.
Frequently Asked Questions
Q1: Is it safe for seniors to take diabetes medications?
Yes, it is safe for seniors to take diabetes medications. However, because seniors are more likely to have other health conditions, it’s important for doctors to consider potential drug interactions and kidney function before prescribing a specific diabetes medication.
Q2: How do I know if my diabetes medication is working?
Regular monitoring of blood glucose levels and periodic HbA1c tests will give an indication of how well your diabetes medication is working. It’s also important to look out for signs of low or high blood sugar levels.
Q3: Can I stop taking diabetes medications if my blood sugar levels are under control?
Diabetes is a chronic condition and stopping medication will likely lead to blood sugar levels increasing again. Always consult with your doctor before making any changes to your medication regimen.
Q4: Can changes in my diet improve my blood sugar levels?
Absolutely. A diet rich in whole grains, lean proteins, and lots of fruits and vegetables can greatly help in managing blood sugar levels. Limiting the intake of processed foods and sugary drinks is also advised.
Q5: Can diabetes be cured?
As of now, there is no cure for diabetes. However, it can be managed effectively with medications, lifestyle changes, and regular monitoring.
ð Related Articles You Might Enjoy
- 5 Breakfast Hacks That Turn Off Insulin Resistance (Eat Before 8am)
- 7 Foods DESTROYING Your Pancreas Every Morning
- 7 Meats You Should NEVER Eat If You Have Diabetes
- 10 Eyesight-Saving Habits for Diabetics (Most People Skip #3!)
ð From Our Health Network:
ð Sources & References
This article is based on information from the following trusted medical sources:
⚕️ Medical Disclaimer
This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or qualified health provider before making changes to your diet, exercise, or treatment plan. The information presented here is based on peer-reviewed research and should not be used for self-diagnosis. If you are experiencing a medical emergency, call your local emergency services immediately.









