⚡ Quick Answer
Diving deep into foot health, we’re introduced to Plantar Warts at the beginning of our list. These are small, fleshy growths that predominantly choose the heels or balls of the feet as their preferred location, precisely where most pressure is exerted.
Diabetes is a condition that affects millions worldwide, posing a plethora of challenges to those diagnosed. Among the many complications associated with diabetes, foot-related issues stand out due to their potential severity and impact on a person’s quality of life. The feet, often overlooked in regular health checkups, can indeed serve as a barometer for one’s overall diabetic health. Not only do they manifest early signs of complications, but they also bear the brunt of long-term diabetes damage. This article aims to highlight ten critical foot complications that every diabetic should be aware of. By understanding these signs and symptoms, one can take proactive measures to ensure better foot health and, by extension, a better quality of life.
10. Plantar Warts
What are Plantar Warts?
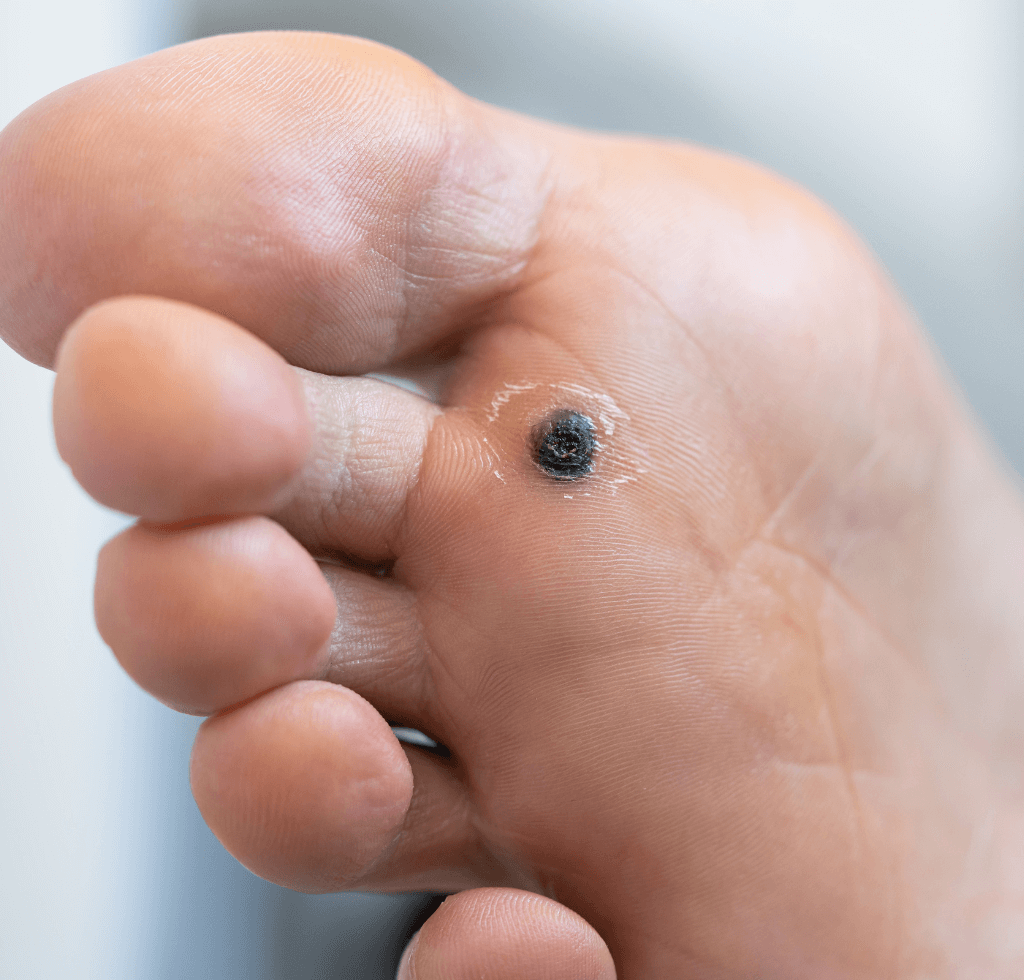
Diving deep into foot health, we’re introduced to Plantar Warts at the beginning of our list. These are small, fleshy growths that predominantly choose the heels or balls of the feet as their preferred location, precisely where most pressure is exerted.
Intriguingly, this very pressure may force plantar warts to grow inward, sheltered beneath a dense layer of skin known as a callus.
Prevalence and Risk
So, how widespread are these unwanted foot residents? The American Podiatric Medical Association reports that plantar warts are the culprit behind about 10% of all foot-related dermatological consultations. And while they can make an appearance on anyone’s feet, those with a compromised immune system, particularly diabetes patients, are more vulnerable.
Diabetes and its Implications
The nexus between diabetes and plantar warts is more profound than just increased susceptibility. Diabetes hampers the body’s inherent ability to heal wounds. Consequently, what might appear as a minor wart to many can spiral into a significant concern for a diabetic. To put things in perspective, the World Health Organization indicates that individuals with diabetes see a 10-20% surge in infection risks, emphasizing the criticality of early detection and intervention.
9. Bunions
Unraveling Bunions
Making their presence known, Bunions claim the next spot on our list. These bony protrusions at the base of the big toe can be quite the eye (and foot) sore. The American Orthopedic Foot and Ankle Society’s data reveals that bunions are an issue for over 23% of 18-65-year-olds, and this figure climbs to 35% for those aged above 65.
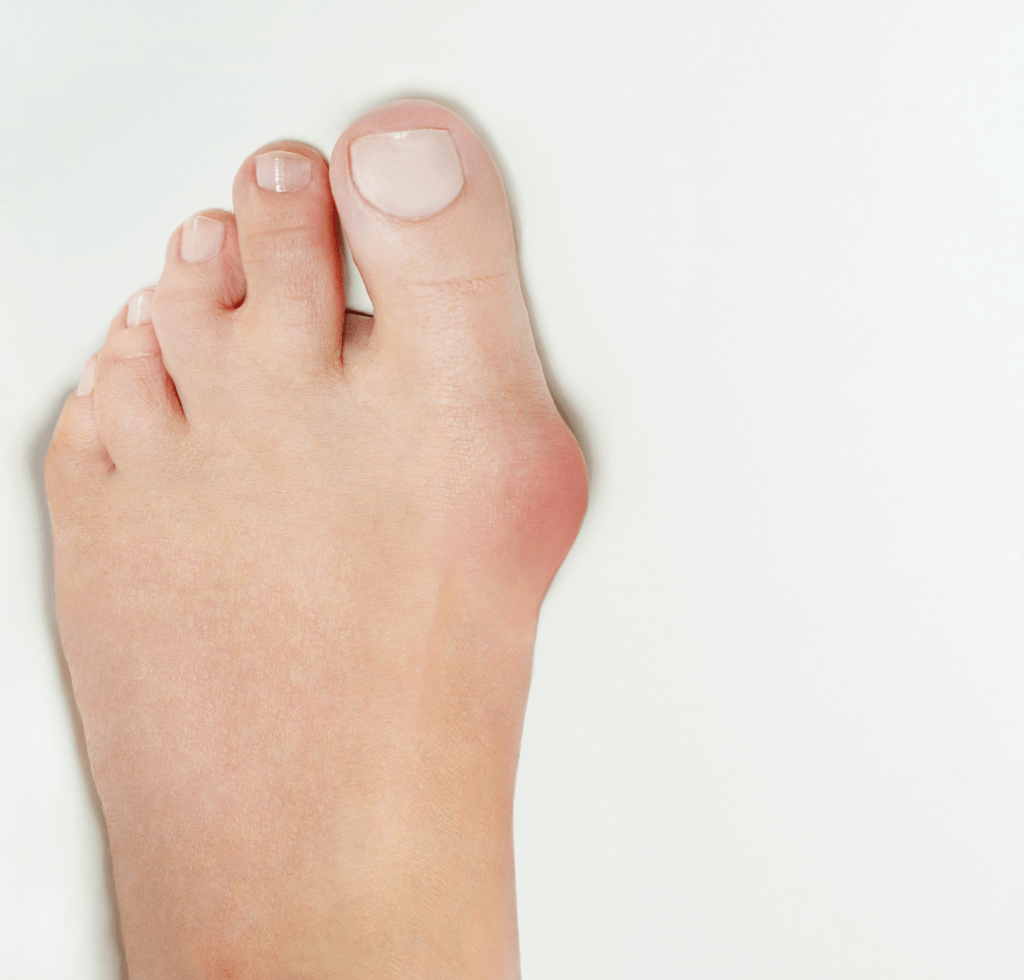
Root Causes
Ever wondered about the origins of these bony bulges? A medley of factors, including genetics, congenital deformities, and foot traumas, can lead to bunions. However, a major contributor is often the shoes we don. Supporting this claim, a survey in the Journal of Foot and Ankle Research discloses that a whopping 68% of respondents wearing poorly-fitted shoes reported foot ailments, with bunions being a prominent complaint.
The Diabetic Dilemma
For most, bunions might just be a painful inconvenience. But for diabetics, the stakes are considerably higher. The toe’s misalignment can usher in secondary complications like ulcers or infections. Underlining the seriousness of this, a study in the Journal of Clinical and Diagnostic Research states that a vast 85% of diabetic foot complications have their origins in minor injuries, the kind that bunions can induce. This brings to the fore the importance of impeccable foot care, encompassing well-fitting footwear and regular foot check-ups, in fending off graver issues.
8. Calluses and Corns
Understanding Calluses and Corns
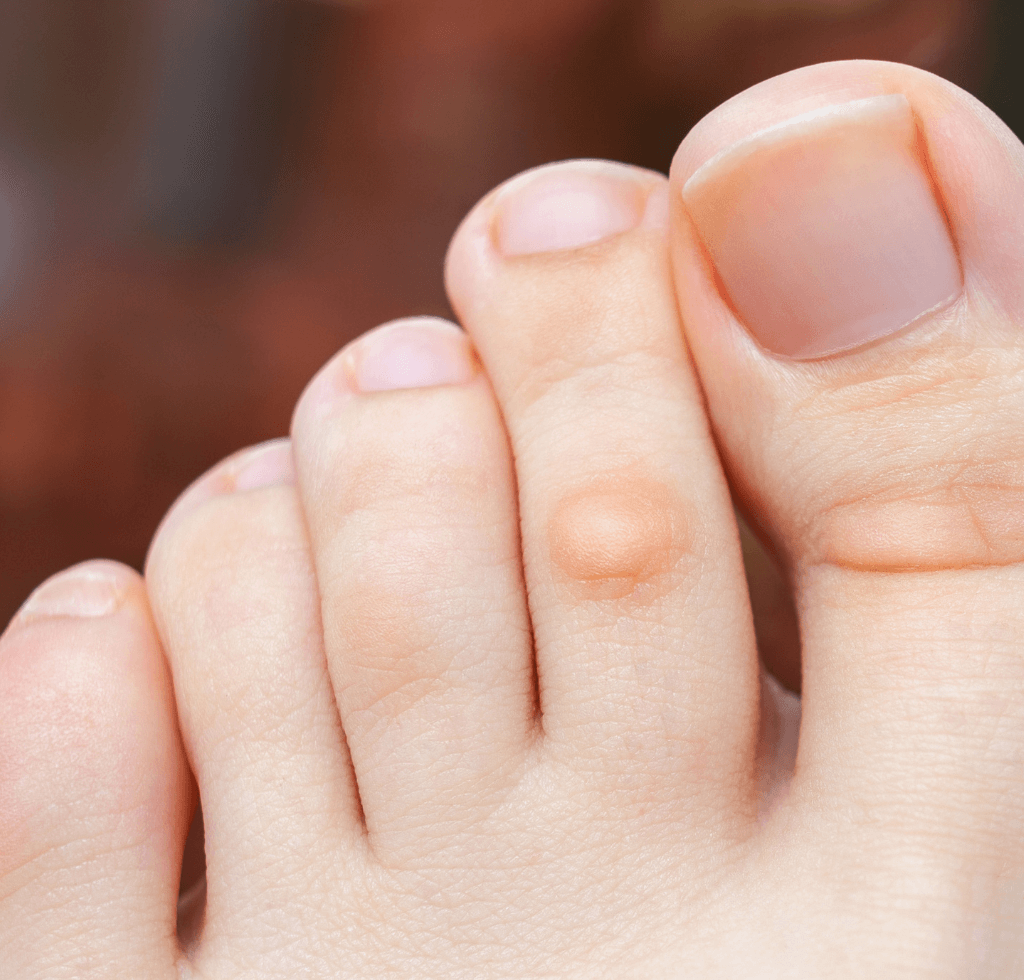
Sliding into the 8th position, we have Calluses and Corns. Our feet, the silent warriors, carry us through our daily routines, often facing the repercussions of our actions. As a defense mechanism against repeated friction and pressure, they develop Calluses and Corns.
These thickened skin patches have become somewhat commonplace, with a survey by the Podiatry Institute indicating that an astounding 80% of adults have faced this issue at least once.
The Diabetic Perspective
Now, while many might brush them off as mere cosmetic nuisances, diabetics need to tread with caution. Beneath the seemingly benign callus, pressure can lead to a breakdown of the deeper skin layers, opening the door to ulcers. This concern isn’t unfounded; a publication in Diabetes Care revealed that roughly one in four diabetics would contend with foot ulcers during their lifetime. Notably, calluses often serve as the unsuspecting precursor.
Delving deeper, the Journal of the American Podiatric Medical Association points out that the risk of foot ulceration skyrockets to three times for diabetic patients harboring corns or calluses. The way forward? Regular consultations with a podiatrist, footwear checks to reduce undue friction, and consistent moisturization can be effective in both management and prevention.
7. Ingrown Toenail
The Sideward Growth
Securing the 7th spot is a condition many overlook until it becomes a literal pain: Ingrown Toenails. Imagine a plant, instead of growing upwards, veering off sideways, encroaching upon its neighbor. In a similar vein, when a toenail forsakes its straight path, opting instead to burrow into the adjacent skin, it’s more than just discomfort we’re talking about.
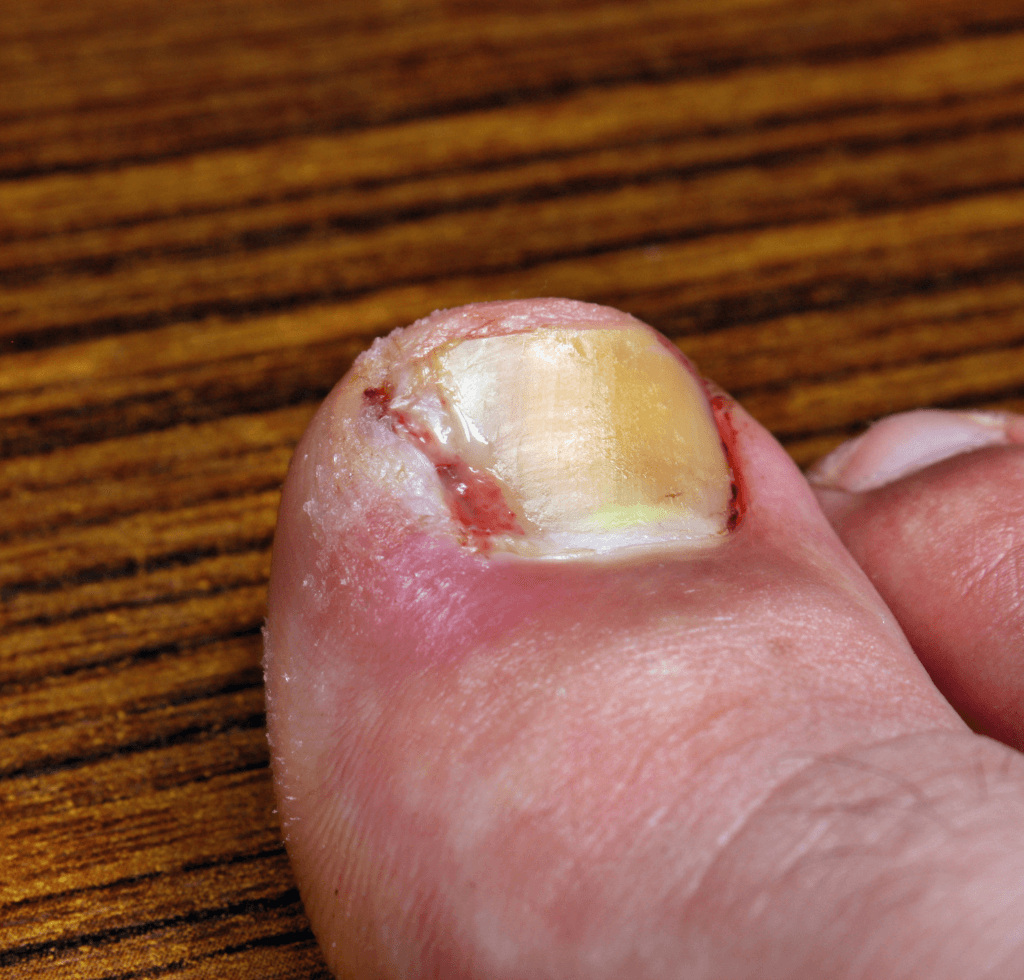
Prevalence and Causes
Ingrown toenails aren’t rare. As cited by the American College of Foot and Ankle Surgeons, their members find themselves treating over 3 million such cases every year. While the misadventure of improper nail trimming often shoulders the blame, a mix of genetics, unexpected trauma, and even certain footwear choices can set the stage for this agonizing ailment.
The Diabetic Complication
Enter diabetes, and the plot thickens. Blending the elements of diminished sensation (neuropathy) with the challenges of wound healing, an innocuous ingrown toenail can quickly become a breeding ground for infections. This isn’t a mere conjecture. A study published in the International Wound Journal highlighted a concerning statistic: of the diabetic patients grappling with foot infections, close to 14% could trace the origin back to complications emanating from an ingrown toenail. The game plan? Maintain impeccable foot hygiene, master the art of proper nail trimming, and at the first sign of redness or swelling, consult a specialist. Prevention, in this case, truly is worth the cure.
6. Dry, Cracked Skin
The Underlying Issue
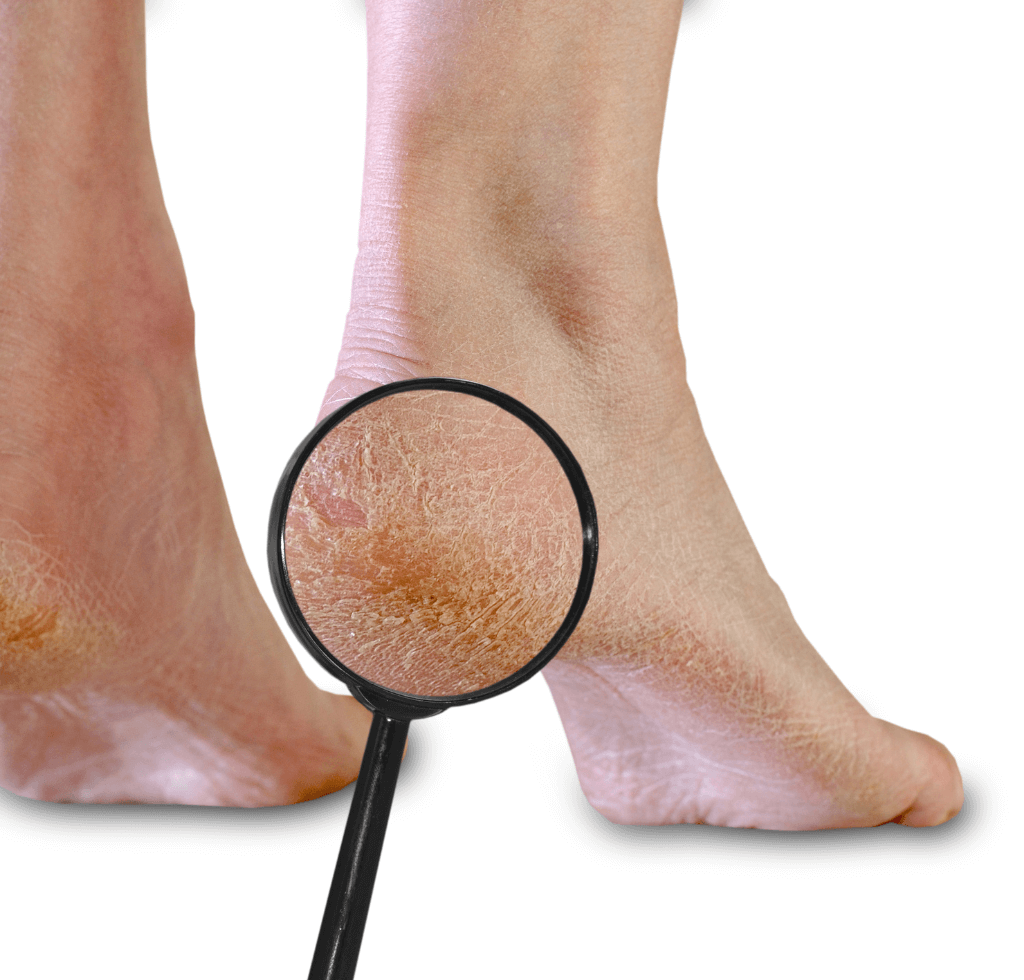
Landing at number 6, we explore a condition often dismissed as merely cosmetic: Dry, Cracked Skin on the feet. Various external factors, such as the environment, choice of footwear, and regular contact with water, can make the skin on our feet susceptible to dryness.
Drawing from the American Dermatology Association’s data, it’s evident that this isn’t a fringe issue – approximately 20% of the U.S. populace grapples with skin dryness, and the feet aren’t exempted.
Diabetes and Its Toll
Introducing diabetes to the equation amplifies the concern multifold. Elevated blood sugar levels have a knack for disrupting the skin’s natural moisture equilibrium, propelling it towards excessive dryness. The fallout? Cracks or “fissures” begin to form, marring the skin’s surface. While these cracks might seem trivial, they’re potential entry points for infections. Highlighting the gravity, a study in the Diabetes Research and Clinical Practice journal unveiled a worrying trend – a significant 30% of minor diabetic foot complications had their genesis in issues tied to dry, cracked skin. The preventive measures? Regular moisturization and meticulous foot care can serve as potent shields against these lurking dangers.
5. Neuropathy
Decoding Neuropathy
Claiming the 5th spot, we delve into Neuropathy. A formidable adversary, Neuropathy, or more specifically, diabetic nerve damage, often chooses the feet as its initial battleground. The symptoms are hard to ignore – a numbing sensation, interspersed with tingling and episodes of pain.

And this isn’t an isolated phenomenon. As per a report from the World Health Organization, a staggering 50% of the global diabetic population is in neuropathy’s grip, manifesting in varying intensities.
The Silent Threat
Neuropathy’s insidious nature lies in the sensory deprivation it inflicts. As sensation diminishes, minor foot injuries, which would otherwise be immediately noticeable, slip under the radar. What starts as an unnoticed bruise or cut can swiftly snowball into graver issues like infections and ulcers. The stakes? The National Institute of Diabetes and Digestive and Kidney Diseases paints a grim picture – a jaw-dropping 60% of non-traumatic lower-limb amputations trace back to diabetes. And neuropathy shoulders a significant part of the blame. The way forward is crystal clear: diabetics must prioritize regular foot examinations and double down on preventive practices.
4. Poor Circulation
Understanding Circulation’s Role
Holding the 4th position is a vital, yet often overlooked aspect of our health: Circulation. At its core, circulation plays the role of a diligent courier, ensuring that every cell receives its quota of oxygen and essential nutrients while simultaneously shuttling away waste products.
However, introduce diabetes into this delicate balance, and we’re faced with potential disruptions. The disease can instigate the narrowing or even blockage of blood vessels, especially in extremities like the feet.
The Diabetes-Circulation Nexus
Drawing from the American Heart Association’s findings, it’s evident that circulatory challenges aren’t mere footnotes in a diabetic’s health journal – a massive 65% of diabetics ultimately succumb to heart disease or stroke, both of which have deep-rooted ties to circulatory disturbances.
What does this mean for the feet? In essence, compromised circulation translates to a sluggish wound healing process and a diminished capacity to fend off infections. Symptoms like cold feet, noticeable discoloration, and unusually prolonged healing durations often signal circulatory issues. Bringing this concern into sharper focus, a study published in the Journal of Diabetes Complications revealed that those with peripheral artery disease (marked by reduced blood flow to the extremities) face a quadrupled risk of developing foot ulcers. The remedy? Embracing regular physical activity, forgoing smoking, and vigilant management of cholesterol and blood pressure can go a long way in ameliorating circulation and curtailing its associated risks.
3. Ulcers
The Insidious Nature of Ulcers
Securing the 3rd spot are Ulcers, deceptive in their appearance and progression. What might begin as a trivial, unnoticed injury or a seemingly harmless blister can evolve into ulcers – persistent open sores that either refuse to heal or recurrently resurface.
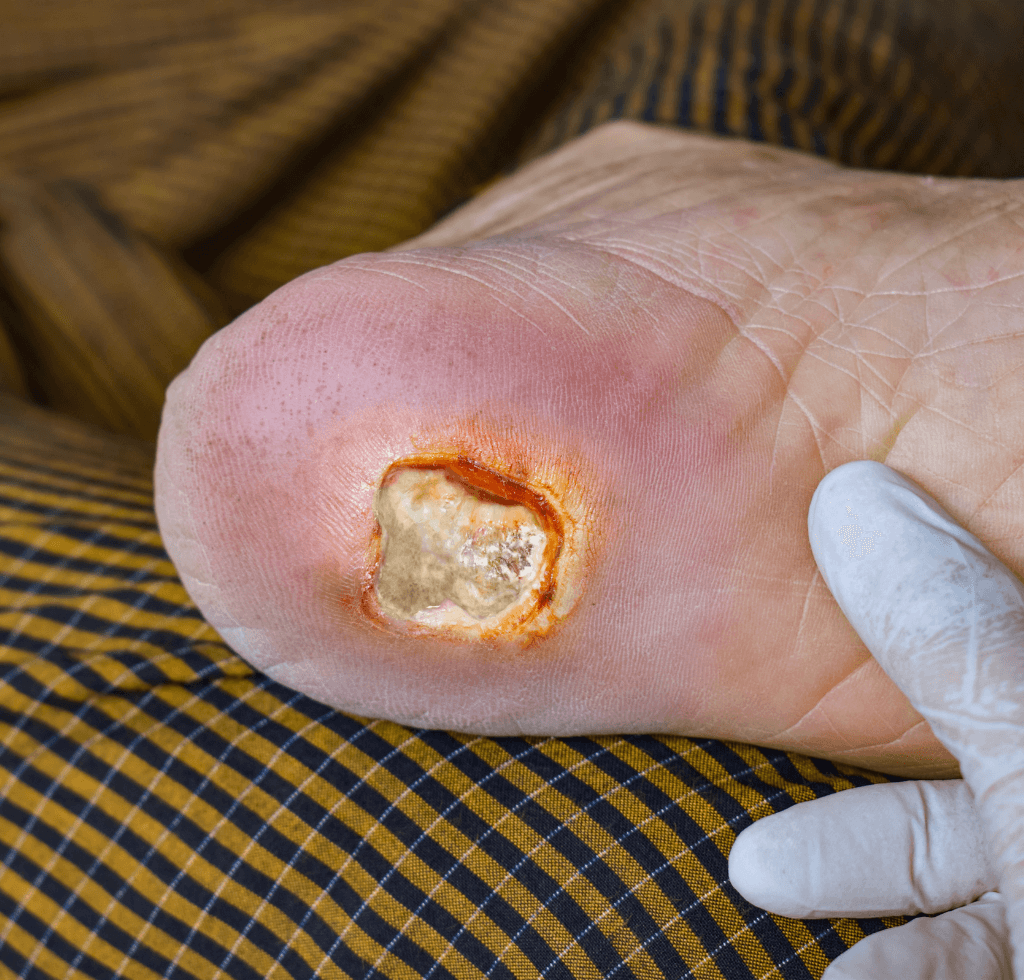
For diabetics, this isn’t a mere superficial issue; the consequences can be profoundly detrimental.
Statistics and Implications
The International Diabetes Federation’s data serves as a clarion call to the severity of the issue: an alarming 10% of diabetics will confront foot ulcers at some juncture in their lives. The depth of these ulcers can be startling, often exposing the underlying tendons or even bones. Given the immune challenges often accompanying diabetes, these ulcers morph into fertile grounds for infections. And if these infections aren’t promptly addressed? They can pave the way for gangrene, and in dire situations, necessitate amputation. The American Podiatric Medical Association adds weight to this concern, pointing out that foot ulcers are the primary trigger for over half of the non-traumatic amputations among diabetic individuals. The countermeasure? A non-negotiable regimen of regular foot examinations, coupled with immediate interventions at the slightest hint of abnormalities.
2. Charcot Foot
Deciphering Charcot Foot

As we progress, we encounter a condition that might not be common parlance but is of grave importance: Charcot Foot. This deformity is birthed from nerve damage, known as neuropathy – an all too familiar nemesis for diabetics.
As the condition advances, the foot’s joints weaken and can collapse under pressure, giving rise to a discernible foot deformity. One might wonder: How can the intricate web of bones and joints in the foot deteriorate without any noticeable external trauma?
Statistics and Implications
Turning to a study in the Journal of Diabetes Complications, we find that while Charcot foot might be on the rarer end of the spectrum, it has been identified in up to 0.5% of the entire diabetic demographic. The stealthy peril here is the desensitization caused by neuropathy. The blunted pain receptors mean that an individual might obliviously continue exerting pressure on a foot that’s already stressed or fracturing. This unwitting persistence can lead to pronounced deformities, and in dire cases, amputation looms as the only feasible recourse. To combat the progression of Charcot foot, timely diagnosis, judicious off-loading (ensuring the foot isn’t bearing weight), and tailored footwear emerge as the linchpins of effective management and treatment.
1. Gangrene
Understanding Gangrene
Reaching the pinnacle of our list, we’re faced with a term that has, for long, been synonymous with dread: Gangrene. The immediate questions that arise are multifaceted – What exactly is gangrene? Why is it held in such trepidation? And crucially, what’s its relationship with diabetes?
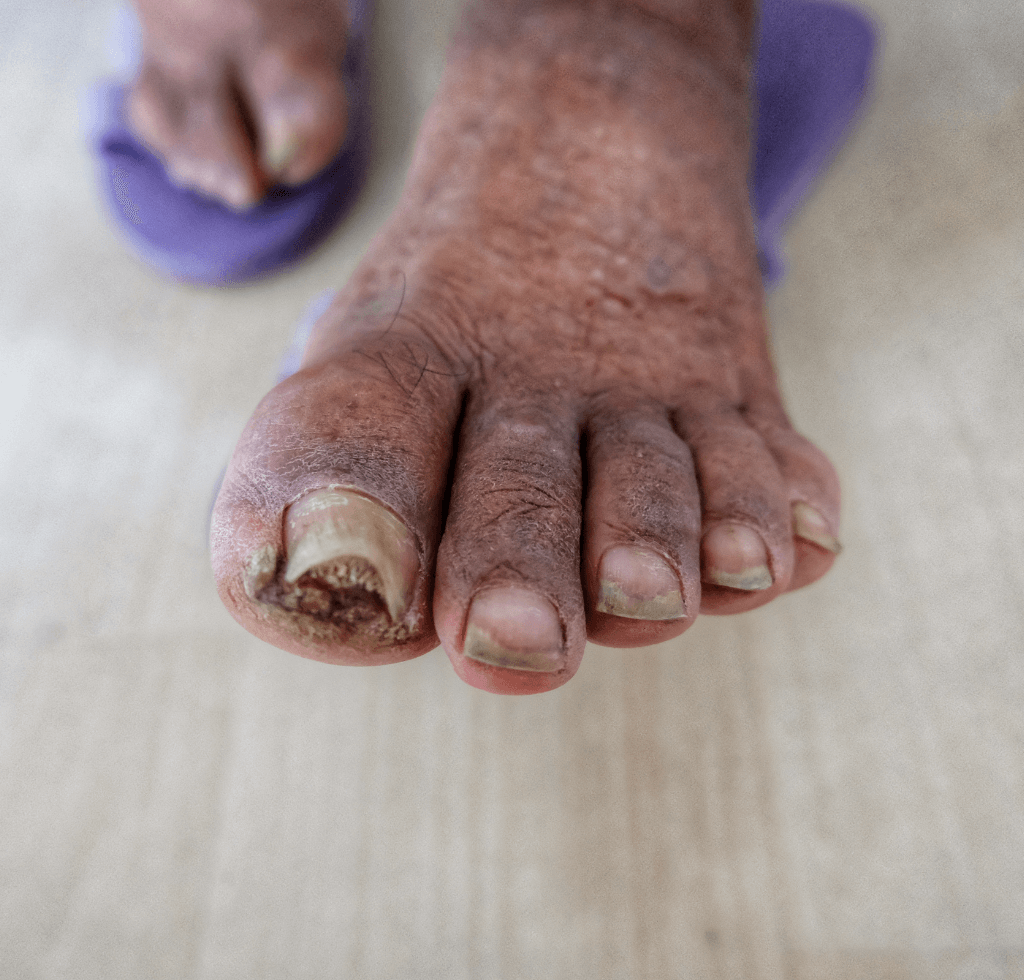
The Mechanics and Impact
Gangrene denotes the demise of body tissue, typically ensuing when there’s an interruption in blood supply or when an infection takes hold. The extremities – fingers, toes, hands, and feet – are the usual hotspots for gangrene. The World Health Organization provides a staggering statistic to underscore its severity: globally, gangrene and the subsequent onset of sepsis contribute to a whopping 40,000 amputations each year. And, alarmingly, a sizeable chunk of these amputees are individuals battling diabetes.
The Diabetic Connection
Diving into the dynamics between diabetes and gangrene, the interplay becomes apparent. Elevated blood sugar levels inherent to diabetes can inflict damage on blood vessels, curtailing blood flow to extremities like the feet. This circulatory challenge, combined with the aforementioned neuropathy, can metamorphose a minor foot injury into a formidable wound, which becomes a magnet for infections and could eventually lead to gangrene. The gravity of the situation is further emphasized by the National Institute of Diabetes and Digestive and Kidney Diseases: diabetics face a risk of amputation due to gangrenous foot that’s a staggering 15 times higher than non-diabetics.
Variants and Solutions
But gangrene isn’t a monolithic entity. It branches out into several types, with dry gangrene emerging as the most frequently diagnosed variant in diabetics. This subtype is characterized by skin that feels cold to the touch, has a dry texture, and undergoes a color transition from brown to a purplish-blue or even black. Early detection can be a game-changer, allowing for halting its advancement and surgically removing the affected tissue. However, left unchecked, gangrene’s implications aren’t just confined to the foot; it becomes a threat to life itself.
In Conclusion: Prioritizing Foot Health in Diabetes Management
Diabetes, with its myriad complications, has long underscored the need for holistic health management. While regulating blood sugar levels remains paramount, the health of one’s feet, often overlooked, is equally crucial. From seemingly benign signs like dry skin to severe indications such as gangrene, the feet can tell tales of the overall health and well-being of a diabetic patient.
These alarming signs are not just mere indicators but are wake-up calls, urging for immediate action and constant vigilance. After all, the key to preventing dire foot complications lies in early detection, prompt treatment, and consistent care.
Don’t stop here. To gain a deeper understanding and visualize these complications, watch our comprehensive video on Diabetes Foot Complications here:
Equip yourself with knowledge and stay one step ahead in your diabetes management journey.
FAQs
- What causes foot problems in diabetics?
Diabetes can lead to various complications due to high blood sugar levels affecting nerves and blood circulation. This can result in issues like neuropathy (nerve damage) and poor blood flow, which are primary contributors to foot problems. - How often should a diabetic person check their feet?
Ideally, diabetics should inspect their feet daily. This routine check helps in early detection of problems like cuts, swelling, blisters, or nail issues, ensuring timely intervention and preventing complications. - Can diabetes foot complications be reversed?
While certain complications like neuropathy cannot be reversed, their progression can be halted or slowed with appropriate care and treatment. Early detection and proper management are essential to prevent irreversible damage. - How can I improve circulation in my feet if I have diabetes?
Regular exercise, maintaining optimal blood sugar levels, avoiding smoking, and massaging the feet can enhance circulation. Consultation with a healthcare professional can provide personalized advice. - Are foot issues a guaranteed complication for all diabetics?
No, foot complications aren’t a guaranteed outcome for every diabetic. However, the risk is higher, making preventive measures, regular foot checks, and appropriate footwear crucial.
📖 Related Articles You Might Enjoy
- 5 Breakfast Hacks That Turn Off Insulin Resistance (Eat Before 8am)
- 7 Foods DESTROYING Your Pancreas Every Morning
- 7 Meats You Should NEVER Eat If You Have Diabetes
- 10 Eyesight-Saving Habits for Diabetics (Most People Skip #3!)
🌐 From Our Health Network:
📚 Sources & References
This article is based on information from the following trusted medical sources:
⚕️ Medical Disclaimer
This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or qualified health provider before making changes to your diet, exercise, or treatment plan. The information presented here is based on peer-reviewed research and should not be used for self-diagnosis. If you are experiencing a medical emergency, call your local emergency services immediately.









